Kitabı oku: «Fat Chance», sayfa 3
Chapter 3
Personal Responsibility versus the Obese Six-Month-Old
Sienna is a one-year-old girl who weighs 44 pounds. She was 10 pounds at birth and was delivered by caesarean section due to her size. Her mother is not obese, but her father is overweight. Her mother tested negative for diabetes during the pregnancy. Since birth, Sienna has had an incredible appetite. Her mother could not breastfeed her because she could not keep up with the baby’s demand for food. An average infant of Sienna’s age will eat one quart of formula per day. Sienna consumed two quarts per day. When Sienna was six months old, we told her mother to start feeding her solid foods. Sienna eats constantly and will scream if her mother does not feed her. She already has high cholesterol and high blood pressure.
Is Sienna obese because of her behavior? Was this learned behavior? When would she have learned this behavior, and from whom? Has she, at age one, learned to control her mother to get what she wants? Should she accept personal responsibility for her actions?
Based on “a calorie is a calorie,” behaviors come first. Personal responsibility implies a choice: that there is a conscious decision leading to a behavior. This behavior is formed because of learned benefits or detriments (e.g., a child placing her hand on a stove and learning it is hot). But does this make sense with regard to obesity? In everyone? In anyone? There are six reasons to doubt “personal responsibility” as the cause of obesity.
1. Obesity Is Not a Choice
The concept of personal responsibility for obesity doesn’t always make sense. In our society today, one has to ask: Are there people who see obesity as a personal advantage? Something to be desired or emulated? Across the board, modern Western societies today value the thin and shun the obese. Obesity frequently comes with many medical complications, and those afflicted are more likely to develop heart problems and type 2 diabetes (see chapter 9). Obese people spend twice as much on health care.12 Studies show that the obese have more difficulty in dating, marriage, and fertility. The obese tend to be poorer and, even in high-paying jobs, earn less than their peers.13
Now ask the same question about children. Did Sienna see obesity as a personal advantage? Did she become obese on purpose? Obese children have a quality of life similar to that of children on cancer chemotherapy.14 They are ostracized by their peers and are the targets of bullies. Many obese children suffer from low self-esteem, shame, self-hatred, and loneliness. One study showed children pictures of potential playmates. Each looked different and some had physical handicaps, such as being deformed or in a wheelchair. The researchers asked the children with whom they would rather play. The obese child came in dead last. Clearly, obesity is not something to which people, especially children, aspire.
However, this view of obesity does not necessarily square with the beliefs of obese people themselves. They see themselves as perpetrators, not victims. They often state that they know their behavior is out of control and that this behavior is their own fault. They frequently experience yo-yo dieting. They lose weight for a period of time, and when they gain it back they blame themselves, seeing the gain as a character failing. They often recount binge eating, which suggests that a degree of dietary control is lost. These experiences of losing control make them think they had the control in the first place. Did they?
2. Diet and Exercise Don’t Work
If obesity were only about increased energy intake and decreased energy expenditure, then reducing intake (diet) and increasing expenditure (exercise) would be effective. If obesity were caused by learned behaviors, then changing those behaviors would be effective in reversing the process and promoting weight loss. Specific and notable successes have led to behavior/lifestyle modification as the cornerstone of therapy for obesity.
There are the anecdotal cases of weight loss by celebrities, such as Kirstie Alley or Oprah Winfrey, who publicly endorse their diets as if they were the latest fashionable handbags. They share their stories on TV and convince their viewers that this lifestyle change is possible for them, too, and that, as with adding the newest fall color to their wardrobe, losing weight will make them attractive and happy. There are reality television shows, such as The Biggest Loser, that document the weight loss (along with many a meltdown) of “normal people” through controlled diet and exercise. Publicity, cash prizes, and constant attention are often enough to change one’s diet and exercise response for a short time. In any magazine and many infomercials, peddlers of new weight-loss remedies provide before and after pictures of people who have lost 100 pounds.
Whether this constitutes a true lasting change in behavior is doubtful. After all, Kirstie Alley and Oprah, celebrities who live in the public eye, have gained their weight back several times (until their newest miracle diet began, countless new diet books were sold, new gurus were anointed, millions of dollars were made, and the cycle repeated itself). There have been numerous reports of contestants on The Biggest Loser regaining much of their weight after the show ended. Most notably, Eric Chopin, the Season 3 winner, appeared on Oprah to tell his sorry tale of gaining at least half the weight back after his victory. He wrote in one blog post, “I’m still not back on track totally. I don’t know what it is.” Significant weight regain has been seen in up to one third of patients who have had surgery for weight loss (see chapter 19), because the reason for the obesity is still there. Unless it’s dealt with directly, regaining will be the norm, not the exception.
Strict control of one’s environment through limiting caloric intake and increasing physical activity can result in weight loss. This is true as long as the environment remains regulated. A perfect example is the army recruit who consistently loses weight due to monitored diet and vigorous exercise. This also accounts for the number of “fat schools” and “fat camps” that have sprung up nationwide. Parents send their overweight child away for the summer and are thrilled when he returns thinner, if harboring parental resentment. There are numerous reports of Hollywood stars who bulk up for a role (remember Robert DeNiro in Raging Bull?) and then lose the excess weight after shooting. (Of course, they have the benefit of round-the-clock personal trainers and nutritionists to monitor their food intake.) While such results are dramatic, they usually cannot be sustained. Environmental control is different from behavioral control (see chapters 17 and 18).
The real problem is not in losing the weight but in keeping it off for any meaningful length of time. Numerous sources show that almost every lifestyle intervention works for the first three to six months. But then the weight comes rolling back.15 The number of people who can maintain any meaningful degree of weight loss is extremely small (see figure 3.1). However, because behavior/lifestyle modification is the accepted treatment, the general explanation of weight regain is that it is the individual’s fault. Because he is “choosing” not to live a healthy lifestyle, the doctors and the insurance industry do not feel it their responsibility to intervene.
The same is true for children. Due to some notable and individual successes, behavior/lifestyle modification is the cornerstone of therapy. However, this is not a winning strategy for most obese children. Research shows that dietary interventions don’t often work. Exercise interventions are even less successful. And unfortunately for children like Sienna, at one year of age they are unable to run on a treadmill. Also, the effects of altering lifestyle for obesity prevention are underwhelming and show minimal effect on behavior and essentially no effect on BMI.

Fig. 3.1. The “Biggest Loser”—Not You. Percentage of obese individuals who were able to maintain their weight loss over nine years.
3. The Obesity Epidemic Is Now a Pandemic
If obesity were just an American phenomenon it would be an epidemic, an outbreak of illness specific to a certain area. One might then blame our American culture for promoting it. Due to our slippage in education and technological superiority, we’re labeled as “fat and lazy” or “gluttons and sloths.” Yet obesity is now a pandemic, a worldwide problem.
The United Kingdom, Australia, and Canada are right behind us. Also, in the past ten years, obese children have increased in France from 5 to 10 percent, in Japan from 6 to 12 percent, and in South Korea from 7 to 18 percent.16 In fact, obesity and chronic metabolic diseases are occurring in underdeveloped countries that have never had such problems before.17 Previously, poorer countries such as Malaysia had problems with malnutrition. Now Malaysia has the highest prevalence of type 2 diabetes on the planet. China has an epidemic of childhood obesity, at 8 percent in urban areas. Brazil’s rate of increase in obesity is predicted to reach that of the United States by 2020. Even India, which continues to have an enormous problem with malnutrition, is not immune – since 2004, the number of overweight children increased from 17 percent to 27 percent. Sienna is not a rarity; her obese peers are being born everywhere. The areas experiencing the greatest rise in obesity and type 2 diabetes include Asia (especially the Pacific Rim) and Africa, which are not wealthy areas.18 No corner of the globe is spared.
This is not an American problem, an Australian problem, a British problem, or a Japanese problem. This is a global problem. Could each of these countries be experiencing the same cultural shifts toward gluttony and sloth that we are? Childhood obesity knows no intellect, class, or continent.
What change in the last thirty years ties all the countries of the world together? As I mentioned in the introduction, the “American diet” has morphed into the “industrial global diet.” Despite people in other countries disapproving of our fast food and TV culture, our diet has invaded virtually every other country. Our fast food culture is now global due to taste, shelf life, cost, shipping ease, and the “cool” factor (a result of effective marketing). Its acceptance is also a response to the contaminated water supplies in these areas: soft drinks are often safer, cheaper, and more available than potable water.19 They are also cheaper and certainly more available than milk.
4. Even Animals Raised in Captivity Are Getting Fat
A recent report documented that, in the past twenty years, animals raised in captivity exhibit increasing body weights. The study examined the records of 22,000 animals of 8 different species, from rats to orangutans.20 These animals were housed in multiple human-built colonies around the world, including labs and zoos. They don’t eat our commercial food. However, their food is still processed and composed of the same general ingredients as our own. Also, these animals drink the same water and breathe the same air that we do. We don’t yet know why this is happening, but the fact that even animals are showing signs of weight gain argues both against personal responsibility and in favor of some sort of environmental insult to which all life on the planet is now exposed (see chapter 15).
5. The Poor Pay More
As stated earlier, personal responsibility implies a choice, usually a conscious choice. Can one exercise personal responsibility if one doesn’t have a choice? It is well known that the poor have much higher rates of obesity and chronic disease than do the rich. There are many reasons for this difference, and it is difficult to pinpoint one factor that is responsible. In the United States the poor exhibit two separate traits that argue against personal responsibility.
First, there are possible genetic issues. It is well known that African Americans and Latinos in the United States are more economically disadvantaged than their Caucasian peers. These demographic groups have higher rates of obesity than Caucasians—40 percent of Latinos and 50 percent of African Americans are obese – and are more likely to have associated medical problems, such as metabolic syndrome.21 Certain genetic variations are more common in specific minority groups. These differences in DNA may, in part, explain the higher rates of obesity and certain metabolic diseases, such as fatty liver (see chapters 7 and 19). Genetic makeup is certainly not a choice.
Second, there are issues of access. There is a difference between the “healthy” diet of the affluent, who can purchase fresh, unprocessed foods that are high in fiber and nutrients and low in sugar, but at high prices, and, the unhealthy diet of the poor, which consists mainly of low-cost processed foods and drinks that do not need refrigeration and maintain a long shelf life. But access does not refer only to what people can afford to buy. Many poor neighborhoods throughout America lack farmers’ markets, supermarkets, and grocery stores where “healthy” foods can be purchased.22 Many supermarkets have pulled out of poor neighborhoods, mainly because of financial decisions based on revenue and fear of crime. The national supermarket chain Kroger, which is headquartered in Cincinati, in 2007 purchased twenty former Farmer Jack stores in the suburbs of Detroit, Michigan, but none within the Detroit city limits. The nearest branch is in Dearborn, eight miles away from downtown. Many who live in low-income areas also have limited access to transportation. Lower-class urban areas throughout America have been labeled “food deserts” because they are unable to sustain a healthy lifestyle. If the only place you can shop is a corner store for processed food, is what you eat really a choice? In wealthier areas of San Francisco, nearly every block has an organic food store, while in the city’s poorer areas, each corner is dotted with a fast food franchise.
Even when all foods are available at low cost, the poor may not have access to refrigerators or even kitchens. Many SROs (single-room occupancy) hotels have only hot plates and no space for keeping or cooking healthy meals. Further, there is the issue of time. Many poor families are led by parents who work multiple jobs and are unable to come home and prepare healthy meals for their children, instead relying on fast food or pizza.
Lastly, the poor suffer from issues of food insecurity. People experience massive amounts of stress when they don’t know where their next meal is coming from (see chapter 6). They eat what is available, when they can – usually processed food. That level of stress is incompatible with the concept of choice. Stressed people can’t make a rational choice, particularly one in which short-term objectives (e.g., sating their hunger) are pitted against longer-term objectives (e.g., ensuring good health).
6. The Greatest Rate of Increase in Obesity Is in the Youngest Patients
When you look at U.S. trends in childhood obesity over the past forty years, you see that every age group is affected. However, the age group that shows the greatest rate of increase in the last decade is the two- to five-year-olds.23 It is impossible to ascribe personal responsibility or free choice to this age group. Toddlers don’t decide when, what, or how much to eat. They do not shop for or cook their own food. However, as all parents know, they do have lungs and they do make their preferences known in the supermarket. Research has shown that children are not able to tell the difference between a TV show and a commercial until they are eight years old. Children in the United States watch an average of three to four hours of TV per day. The programs are interspersed with commercials that target these young viewers and convince them of what they need.24 If you can’t discern what’s marketing and what’s not, how can you defend yourself against it?
We even have an epidemic of obese six-month-olds.25 They don’t diet or exercise. They drink breast milk or formula and lie in their cribs. While our society easily puts the blame on our current diet and exercise practices, how does this explain the obese six-month-old? Whatever theory you have to explain the obesity epidemic, it has to explain them also. The concept of diet and exercise in an obese infant is a non sequitur. Sienna and other obese six-month-olds lay waste to the idea of personal responsibility for obesity. Instead of perpetrator, the obese six-month-old must be a victim. But a victim of what? Or whom?
Who Is to Blame?
So we are left with a conundrum. We’re all eating more and exercising less. By 2050, obesity will be the norm, not the exception. Do abnormal behaviors drive obesity? If so, behavior is primary, behavior is a choice, and personal responsibility is front and center. But what if it’s the other way around? What if our biological process of weight gain drives these abnormal behaviors (see chapter 4)? To argue against personal responsibility is to argue against free will. “Free will” is defined as “the power of making free choices that are unconstrained by external circumstances or by necessity.” Who is making the choices? Philosophers and scientists have argued this topic for centuries. Albert Einstein stated, “If the moon, in the act of completing its eternal way around the earth, were gifted with self-consciousness, it would feel thoroughly convinced that it was traveling its way of its own accord…so would a Being, endowed with higher insight and more perfect intelligence, watching man and his doings, smile about man’s illusion that he was acting according to his own free will.” Anthony Cashmore of the University of Pennsylvania recently proposed that free will was in reality an interaction between our DNA and our environment, along with some stochastic (random) processes.26 Because our DNA cannot be changed, and because random processes are random, we’re left with our environment, both as the sentinel exposure and the only factor than can be manipulated.
The debate about who or what is to blame for obesity will not be settled anytime soon. But I would argue that ascribing personal responsibility to the obese individual is not a rational argument for an eminently practical reason: it fails to advance any efforts to change it. The obesity pandemic is due to our altered biochemistry, which is a result of our altered environment. Part 2 will demonstrate how our behaviors are secondary, and are molded by our biochemistry.
PART II
To Eat or Not to Eat?
That’s Not the Question
Chapter 4
Gluttony and Sloth – Behaviors
Driven by Hormones
Marie is a sixteen-year-old girl with a brain tumor of the hypothalamus (the area at the base of the brain that regulates the hormones of the body). When she was ten, cranial radiation was required to kill the tumor. Since then, she has gained 30 pounds per year; she weighed 220 pounds when I first saw her. Her insulin levels spiked to incredible heights every time she ate. She had a form of intractable weight gain due to brain damage called hypothalamic obesity. She wouldn’t do any activity at home, couldn’t study in school, and was severely depressed. As part of a research study, I started her on a drug called octreotide, which lowered her insulin release. Within one week Marie’s mother called me to say, “Dr. Lustig, something’s happening. Before, we would go to Taco Bell where she would eat five tacos and an encharito and still be hungry. Now we go, she has two tacos and she’s full. And she’s starting to help me around the house.” After beginning the medication, Marie commented to me, “This is the first time my head hasn’t been in the clouds since the tumor.” Within a year, she was off antidepressants and had lost 48 pounds.
Who’s at fault here? Is this a case of free will? And what happened to cause Marie’s reversal? If obesity is truly a result of too much energy intake (gluttony) and too little energy burned (sloth), then my last sixteen years taking care of obese children has been a complete and utter waste. Because it’s become painfully evident, after years of motivating, pleading, and arguing, that I can’t change children’s behavior. And I certainly can’t change their parents’ behavior. It was this insight from Marie, and other children like her, that exposed the inherent problems in our current thinking. Biochemistry and hormones drive our behavior.
The idea that biochemistry comes first is not a new one, but it is one that physicians, scientists, and the public should embrace. Think about the following: You see a patient who drinks ten gallons of water a day and urinates ten gallons of water a day (highly abnormal). What is wrong with him? Could he have a behavioral disorder and be a psychogenic water-drinker? Could be. Much more likely he has diabetes insipidus, a defect in a water-retaining hormone at the level of the kidney. You see a twenty-five-year-old who falls asleep in his soup. Was he up partying all night? Perhaps. But he may have narcolepsy, which is a defect in the hormone that stimulates arousal (orexins) in the midbrain. The biochemistry drives the behavior. Schizophrenia for one hundred years was a mental health disorder. Now we know that it’s a defect in dopamine neurotransmission and that no amount of psychotherapy is going to help until you treat the biochemical defect. Thus, we routinely infer “biochemical” defects in many “behavioral” disturbances.
Introducing Energy Processing and Storage
To appreciate how hormones control eating behavior, first we have to look at what happens to the food we eat. In response to various brain signals (hunger, reward, stress) we ingest various calorie-laden foodstuffs (combinations of fat, protein, carbohydrate, and fiber, with some micronutrients thrown in for good measure) to build muscle and bone for growth and/or to burn for energy. These calories arrive at the stomach, a muscular bag in the abdomen about the size of a baseball glove, which releases hydrochloric acid, to begin to digest the food into smaller components. The food makes its way into the next part of the digestive tract, called the small intestine. There, a bunch of enzymes (proteins) digest the food into even smaller components, such that dietary fats are digested into fatty acids, dietary protein is sliced into amino acids, and carbohydrate is cleaved into simple sugars (mostly glucose, with varying amounts of the sweet molecule fructose). But we can’t digest dietary fiber, so it remains intact. The fiber speeds the rate of transit of the food through the small intestine (see chapter 12), while limiting the rate of absorption of the other nutrients.
Once absorbed in the small intestine, the amino acids and simple sugars travel via the portal vein to the liver for immediate processing. The fatty acids are transported to the liver by a different route (the lymphatic system). The liver has first dibs on the processing of each of these three classes of nutrient. Whatever the liver can’t take up appears in the general circulation. Rising levels of glucose or amino acids or fatty acids reach the pancreas, where the beta-cells release the hormone insulin.
Insulin, in common parlance, is known as the diabetes hormone. Diabetics inject insulin to lower their blood glucose. But where does the glucose go? To the fat. Insulin’s actual job is to be your energy storage hormone. When you eat something (usually containing some form of carbohydrate), your blood glucose rises, signaling the pancreas to release insulin commensurate with the rise in blood glucose. (This is the theory behind the concept of glycemic index, which is discussed in chapter 17.) Insulin then tops off the liver’s energy reserve by making liver starch (called glycogen), and shunts any amino acids from the blood into muscle cells. Excess fatty acids, or blood lipids, are cleared into fat cells for storage for a “rainy day,” where they get turned into greasy triglycerides (such as the fat surrounding your steak). There is no energy storage without insulin – it is the key that unlocks the door to the fat cell to let energy enter and subsequently be stored as fat. Insulin makes fat – the more insulin, the more fat. And there it sits…and sits…as long as there is insulin around. When the insulin levels drop, the process goes in reverse: the triglycerides get broken down, causing the fat cells to shrink – when it happens, that’s weight loss! – and the fatty acids reenter the bloodstream and travel back to the liver, where they are burned by the liver or other organs. In this way, by cycling our insulin up and down, we burn what we need, and store the rest.
Introducing the Hypothalamus
For the past sixty years we’ve known that the brain, especially the one cubic centimeter at the base of the brain called the hypothalamus, controls this process of energy balance. It’s about the size of a thumbnail, and it is “ground zero” for the control of almost all the hormonal systems in the body.
Imagine the organization of a taxicab company. At the bottom are the taxicab drivers, getting their orders from a central dispatcher by radio and shuttling passengers all over town. The target organs – the thyroid, the adrenal, the testicles, the ovaries – are like the cabbies. They receive their orders from the central dispatcher, or, in this case, the pituitary or “master gland,” which acts as the main control system. The hormones released are similar to the taxi’s computerized system, signaling to the pituitary to tell it how things are going out in the field. Like the central dispatcher who directs the cabs based on their location, the pituitary will then adjust its message.
However, there is another layer of control: the chief executive officer, or CEO, who decides on hiring and firing, contracts, upgrades, and mergers and acquisitions. The company can’t turn a profit without the cabbies, be efficient without the dispatcher, or be sustainable long term without a CEO. Furthermore, the CEO can alter the direction of the company based on the profitability of its cabdrivers. The CEO is akin to the hypothalamus. It sends blood-borne hormonal signals to tell the pituitary what to do. It then makes large-scale decisions based on the function of the peripheral glands, which send it information via the bloodstream. And it integrates information from other areas of the brain to alter the long-term hormonal milieu. Marie’s hypothalamus was damaged beyond repair, which caused it to be ineffective in controlling her hormones and, therefore, her behavior.
The Ventromedial Hypothalamus (VMH) and Energy Balance
The hierarchy of energy balance is even more complicated. A subarea of this thumbnail is called the ventromedial hypothalamus (VMH), which serves the executive function of controlling energy storage versus expenditure. Because energy balance is so important to survival, there are redundant systems in case one goes amiss to ensure that the organism doesn’t die. It’s clear that energy balance is the most complex function we humans perform. It’s likewise apparent that energy storage, or the creation of fat cells, is the default strategy. Bottom line, we humans won’t give up our hard-earned energy without a fight.
There are afferent (incoming) and efferent (outgoing) systems that control energy balance27 (see figure 4.1). The VMH receives acute meal-to-meal information from the GI (gastro-intestinal) tract on both hunger and satiety (not shown in the figure). Either one can turn the feeling of hunger on or off by itself. But that’s not all. In addition, the VMH receives more long-term information on one’s fat stores and nutrient metabolism: in other words, whether your body needs to consume more calories for longer-term survival. This information is conveyed via the hormones leptin and insulin to the hypothalamus, where it is decoded and either stimulates or suppresses appetite, and adjusts energy expenditure accordingly.
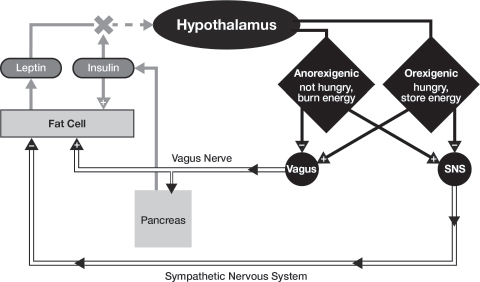
Fig. 4.1. How the Brain and Hormones Work Together (or Don’t) to Regulate Energy Balance. The hypothalamus receives hormonal information from the fat cells (leptin). This information is processed into one of two signals: (a) anorexigenesis (I’m not hungry and I can burn energy) or (b) orexigenesis (I’m hungry and I want to store energy). Anorexigenesis turns on the sympathetic nervous system (responsible for muscle activity and fat loss), and turns off the vagus nerve (responsible for appetite and fat gain); while orexigenesis does the opposite. However, high insulin blocks the leptin signal, mimicking “brain starvation” and driving orexigenesis, so that we feel hungry even when we have eaten.
From there, the hypothalamus sends signals from the brain to the body via two components of the autonomic nervous system. The autonomic nervous system is that portion of your body that controls your heart rate, blood pressure, and energy metabolism without your conscious effort. It is composed of two parts: the sympathetic nervous system (responsible for the fight-or-flight response) and the parasympathetic nervous system (responsible for “vegetative” functions such as food absorption and energy storage). The vagus nerve is one of the key components of the parasympathetic nervous system. There is a delicate balance and feedback loop between the sympathetic and parasympathetic systems. When that balance changes, that’s when problems ensue.
The vagus nerve is fascinating. It connects the brain to all the digestive organs in the abdomen: the liver, the intestine, the pancreas, and also to the fat cells. It performs many different functions but with one ultimate goal: to store energy. The vagus is your energy storage nerve. The vagus has two parts: the afferent part (organs to brain), and the efferent part (brain to organs). The afferent vagus communicates the sensation of hunger between the stomach and brain, and also communicates information on energy processing during a meal between the liver and brain. The VMH interprets all these afferent signals, which leads to one of two physiologic states: anorexigenesis (I don’t need any more food, I can burn energy as needed, and I feel good) or orexigenesis (I don’t have enough food, I don’t want to burn any energy, and I will feel lousy until I get some more).
